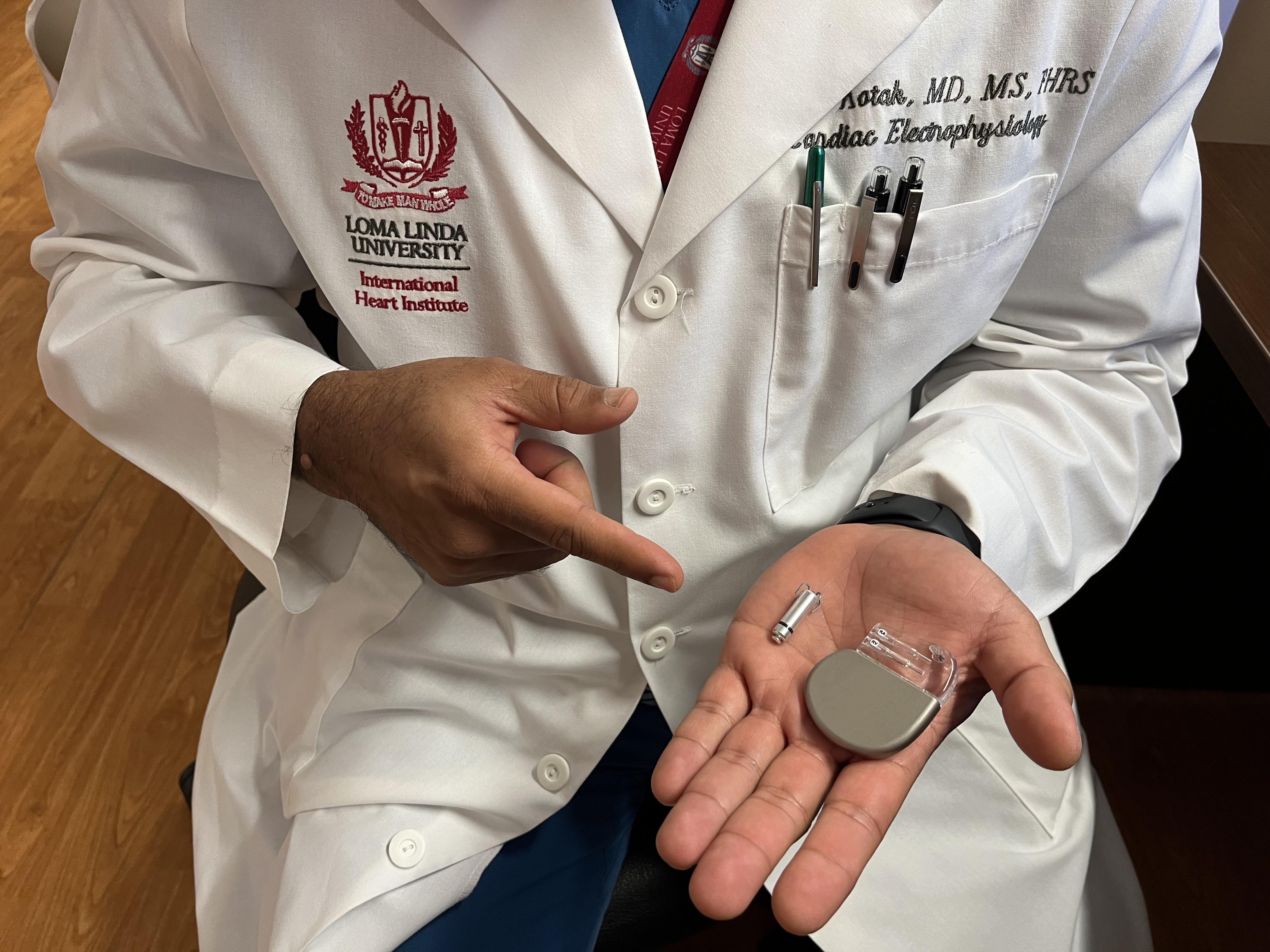
Cardiac electrophysiologist Dr. Kamal Kotak demonstrates where a leadless pacemaker would insert into the human heart.
Advancements in pacemaker technology are opening new doors for patients, says Kamal M. Kotak, MD, a cardiac electrophysiologist at Loma Linda University International Heart Institute. He and experts at the International Heart Institute are leaders in the region for implanting the latest FDA-approved pacemakers, which lower patients’ risk for medical complications and offer more precise, personalized solutions for managing heart rhythm disorders.
Pacemakers help support the heart's electrical system, which controls the heartbeat, says Kotak. Electricity in the heart begins in a group of cells at the top of the heart and spreads to the bottom, causing the heart to contract and pump blood. He says aging, heart muscle damage, and certain genetic conditions can cause a slowing of heart rhythm that may require a pacemaker — a small device implanted in the chest with wires (leads) connecting to the heart to prevent it from beating too slowly.
New pacemaker techinques, such as leadless pacemakers and cardiac conduction system pacemakers, achieve what traditional pacemakers can by sending electrical signals to help the heart beat properly while offering a more tailored fit to patients.

Kotak compares and contrasts different pacemakers' features, including size, shape, and capability.
The leadless pacemaker is self-contained, Kotak says, meaning that, unlike traditional pacemakers placed in a patient's chest with leads connecting to the heart, leadless pacemakers are implanted directly into the heart’s right ventricle by minimally invasive method — without cuts or stitches. While the leadless pacemaker is not for everyone, Kotak says there are specific scenarios where it can be used instead of a traditional pacemaker. He says the traditional pacemaker remains the standard method of pacing the heart.
Conduction system pacemakers, also called left bundle branch area pacemakers (LBBAP), are the newest on the scene, Kotak says. He says that its design helps the heart's electrical signals move in a more coordinated and natural way with one wire instead of several. This feature spares patients from dyssynchrony, a condition that may develop in up to 15% of patients with traditional pacemakers experience. It can lead to severe weakening of the heart or symptoms of heart failure. In addition, Kotak says LBBAP serves as an alternative and at times a superior option for a select group of patients who need cardiac resynchronization therapy.
Louise Correnti, 76, received a cardiac conduction system pacemaker in June, restoring her health. She first noticed her shortness of breath in April when performing everyday activities, such as walking her dogs in Beaumont. She says she was surprised by this symptom, given she attends Pilates four days a week and has been an avid motorcycle rider for three decades.
After a few weeks of her smartwatch logging low heart rate, Correnti contacted her care team at Loma Linda University Health (LLUH). Within days, Correnti met with International Heart Institute experts who remotely monitored her heart using a wearable harness device and determined the next steps.
Read: Using smart wearables to your heart’s advantage
“I was impressed with how swiftly the LLUH care teams moved,” says Correnti, who was out running errands when she received a call saying she needed a pacemaker that day.

Correnti has been an avid motorcycle rider for three decades and enjoys multi-day trips throughout the Southwest.
Kotak says Correnti had a complete heart block, meaning the electrical impulses that control the heartbeat fail to pass between the top and bottom chambers of the heart. A complete block can affect blood flow to the body and brain, leading to complications including fainting with injury, low blood pressure, damage to internal organs, and cardiac arrest.
Correnti says she didn’t fully grasp the gravity of her condition at the time but is thankful that Kotak and the team saved her life with the conduction system pacemaker. A retired esthetician, Correnti embraces her active lifestyle and even started playing pickleball after recovering from her procedure. She continues to travel by motorcycle or plane (she recently visited Cancun) while keeping an eye on her home monitor connected to her pacemaker.
Though a remote monitoring program, Kotak says he and his team use an advanced software to keep track of patients’ heart rate, heart rhythm, and pacemaker activity. Monitors alert patients and their care teams of any unusual activity and issue an early warning for any malfunction.
“Our care teams can leverage advances in pacemaker and remote monitoring technology to optimize care for people like Mrs. Correnti,” Kotak says.
At Loma Linda University International Heart Institute, physicians are committed to providing patients with personalized and comprehensive cardiovascular care. To learn more, please visit lluh.org/heart-vascular or call 909-558-7717 to make an appointment.



