18-year-old Abigail Aguilar overcame extremely rare autoimmune disorder – only 21 cases ever reported in pregnant women.
Pregnant, hallucinating, misdiagnosed, and misunderstood. Abigail Aguilar was 18 years old when she found out she was pregnant and began experiencing extreme symptoms. She was unsure if they were normal and was cast aside by various medical facilities in the southern central valley. Through a multidisciplinary approach to her case, experts at Loma Linda University Health diagnosed Aguilar with anti-NMDA receptor encephalitis, a neurologic disease caused by the body’s production of antibodies that attack a receptor in the brain causing inflammation. She was gifted a normal future by those who extinguished the fire in her brain.
I was going to get out of the never-ending hell of being a prisoner to my own mind.
Abigail Aguilar
Once Aguilar came to terms with the idea of being a mom at 18, she began feeling the physical effects of pregnancy. Morning sickness and migraines lead to weekly emergency department visits in her hometown, eventually leading to a diagnosis of intense morning sickness. But something was still off.
“I felt as if something was being overlooked, but I was just an 18-year-old girl, not a licensed professional. How was I to explain that?” Aguilar said.
She quickly fell into depression and struggled with short-term memory loss and hallucinations. She often thought, “How could nothing be wrong?”
Aguilar often had inappropriate outbursts and was labeled obnoxious. She would stare blankly into space for minutes and began feeling afraid of people and things that were typically comforting. She even began viewing her mother as an imposter. The woman looked like her and acted like her, but in Aguilar’s head, the person was a character playing the part of her mother and was someone she couldn’t trust. For months, this is how the isolated Aguilar felt about everyone around her, and she thought it was her versus the world. Realistically, it was Aguilar versus her brain.
An emergency nurse at a medical facility in Kern County suggested that Aguilar seek help from Loma Linda University Health, two hours away from home. Finally being taken seriously, Aguilar was admitted and was treated at Loma Linda University Health for two months.
Initial tests came back normal, but experts knew her case was far from normal. Aguilar was now confused, angry, and hallucinating, and had to be restrained for her safety. Mark Ard, MD, a clinical ethics consultant and medical director of psychiatric consultation and liaison services, observed her psychosis and staring spells, spoke with her mother, and quickly understood this was not a normal presentation of psychosis.

“When she first came to us it was thought she needed to go to a psychiatric hospital. But I was worried because the timeline of her condition, age, and understanding that she was once high functioning did not fall in line with usual psychiatric conditions,” Ard said. “Multiple medical conditions can present with psychiatric symptoms, and the team began searching when we decided there had to be a physical reason.”
A lumbar puncture finally provided answers — brain inflammation, specifically anti-NMDA receptor encephalitis.
“I then knew I was going to get out of the never-ending hell of being a prisoner to my own mind,” Aguilar said.
Doctors informed her that anti-NMDA receptor encephalitis and the inflammation and damage can cause a variety of symptoms like cognitive dysfunction, seizures, and mood and behavioral changes.
While Aguilar finally had answers, there was now a new discovery to be made: What caused this rare encephalitis in her brain?
Chair of neurology, Travis Losey, MD, says various infections and viruses can cause inflammation but it is primarily found in those with gynecological cancers.
“The core problem is the abnormal autoimmune response, and understanding the cause of it is essential to treatment,” Losey said. “We began searching for cancers and infections.”
The cancer team at LLUH found a tumor and a cyst on her left ovary, the trigger of her brain inflammation. Aguilar was rushed to surgery to have the tumor, cyst, and ovary removed.
After surgery, Aguilar’s condition continued to worsen. That prompted physicians to extensively research materials to ensure Aguilar was receiving the best treatment. Her team discovered that in rare cases pregnancy can exacerbate the condition.
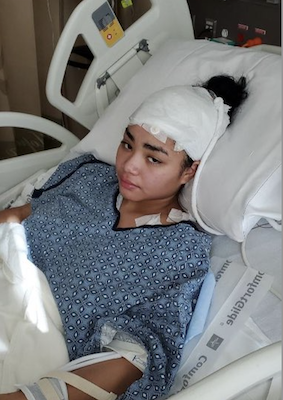
It became clear to doctors that only Aguilar or her baby would survive treatment.
A multidisciplinary team then conferred to hold a considerate and cautious discussion regarding Aguilar’s case with the clinical ethics committee.
“We were constantly researching literature and reviewing external case reports,” Ard said. “The medical team and Abigail’s family tirelessly discussed the risk of treatments on the baby, and the risk of the pregnancy in Abigail.”
Recovering from surgery, and in a poor physical and mental state, doctors determined Aguilar wasn’t medically capable of making the decision.
“My mother is someone who I have and always will hold in high regard for everything she did for me,” Aguilar said. “She was the one with the final say and chose me.”
Aguilar’s pregnancy was terminated, and her health improved drastically. She began eating and walking and grew more conscious each day. She began growing in social skills with the hospital staff at which she once had outbursts and welcomed medical students to study her case and ask her questions.
In February of 2022, Aguilar learned she could finally go home but would carry her disease for life. Anti-NMDA receptor encephalitis requires ongoing treatment and follow-up with a neurologist specializing in autoimmune disorders. The long-term treatment includes immunotherapy agents like steroids and IV treatments.
Aguilar leans on her mother and family to distinguish which memories are real and which were hallucinations. Pieces of her personality that were subdued by the inflammation have returned, while other traits were symptoms of the inflammation and are gone with it. Feeling fully conscious for the first time in months, Aguilar began feeling angry, and pitiful and questioned why this happened to her.
“I had to realize that I went through something that is sure to leave a deep scar, but I had to embrace my scars rather than hate them,” Aguilar said. “They’re a part of me now and although it's a work in progress, I’m doing it. I’m embracing my scars and seeing them as a symbol of my strength, not weakness.”
The multidisciplinary approach that was used to treat Aguilar is an everyday practice at Loma Linda University Health. Learn more about some of the service lines involved: Neurology, Obstetrics and Gynecology, Behavioral Health, Cancer Center.