
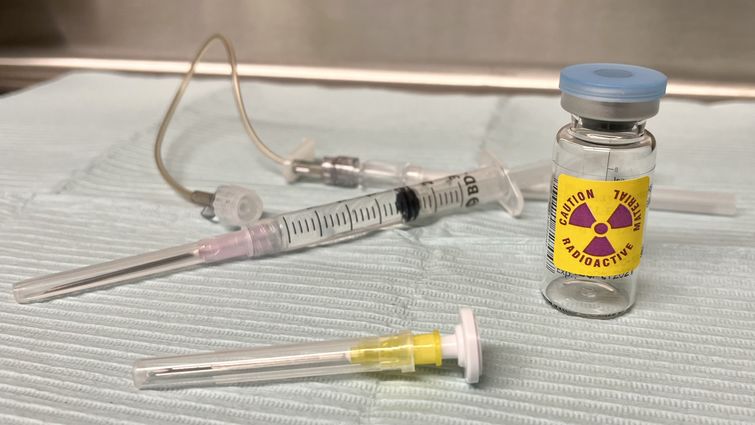
Equipment used to administer radioactive iodine therapy to treat patients' thyroid disorders or thyroid cancers.
Radioactive iodine therapy (also called RAI or I-131) is the oldest form of radiation therapy used to treat humans, yet many people may not be familiar with the treatment until advised to undergo it themselves, says Eric Peters, MD, a radiologist at Loma Linda University Cancer Center. For January’s Thyroid Awareness Month, Peters discusses the basics and benefits of radioactive iodine therapy.
“Awareness of radioactive iodine therapy now can save you a lot of the stress and pressure from only discovering it in the future if you or a loved one have been diagnosed with a thyroid cancer or disorder and emotions are running high,” Peters says.
Radioactive iodine therapy uses the radioactive isotope iodine-131 to target and destroy tissue in the thyroid gland — the major organ in the body that takes up and holds onto iodine. Peters says providers may refer patients with thyroid disorders such as hyperthyroidism or Graves Disease to undergo this therapy. Additionally, he says patients with papillary or follicular thyroid cancer may receive the treatment after having had all or part of their thyroid removed in surgery. The therapy destroys thyroid tissue not removed by surgery and treats any thyroid cancer cells that spread to lymph nodes and other body parts.
“Thyroid cancer tends to grow slowly, and even after surgical removal of the thyroid, lingering thyroid cancer could be affecting lymph nodes that are as small as one millimeter in size,” Peters says. “Because the surgeon’s chance of finding all the tiny affected lymph nodes is low, radioactive iodine therapy is the best way to target thyroid cancer that has spread to the bones, lungs, or other areas.”
Read: Five things to know about thyroid cancer
Since the iodine is radioactive, Peters says it decays over time and releases little bits of energy that damage whatever tissue surrounds it. In cases where many iodines are next to each other within thyroid cancer, the radioactive iodine can destroy the cancerous cells.
Peters says iodine-131 therapy provides two benefits for patients: precision and staging for cancer. The treatment contains subatomic particles called beta particles that travel only a millimeter or two in humans, causing it to target and damage specific areas with high iodine concentrations such as thyroid tissue and thyroid cancer. The therapy also emits a gamma ray that travels outside the body and creates an invisible light source. Imaging detects the gamma rays, and experts interpret the scans to determine the stage of thyroid cancer.
If you can drink water through a straw, you can get this therapy.Dr. Eric Peters
Peters says receiving radioactive iodine therapy is relatively seamless for patients at Loma Linda University Health. Most patients with thyroid disorders will receive the treatment orally through a syringe, followed by a cup of water. Thyroid cancer patients who receive larger dosing of the radioactive iodine will drink the solution through a small clear tube, followed by a cup of water. The iodine is clear and tastes just like water, Peters says.
“If you can drink water through a straw, you can get this therapy,” he says.
Brie Wienhoff, MSRS, CNMT a nuclear medicine supervisor in LLU’s radiology department, says her experience receiving radioactive iodine therapy to treat hyperthyroidism at the age of 16 prompted her to look into the nuclear medicine field as a future career.
“It seemed like a different world, a less invasive way to image, diagnose, and treat the body,” she says “I view the iodine 131 therapy as bridge that was used to get me back to my normal self.”
Before the therapy, Wienhoff says she felt sapped of energy and lived her teenage life in “slow motion.” The therapy ended Wienhoff’s symptoms by radiating the thyroid tissue and treating her hyperthyroidism. Like many other patients after receiving the therapy, Wienhoff takes daily thyroid hormone medication to help the thyroid’s metabolism.
“It truly is a full circle experience to now be other side of these exams and help patients travelling down the same path I had,” she says. “I can honestly empathize with patients’ questions, concerns, anxiety, and fear.”
Many patients undergo radioactive iodine therapy just once; others may repeat the treatment at personalized time intervals. After swallowing the radioactive iodine, Peters says patients become radioactive for a certain period of time, depending on dosing. Therefore, Peters advises consulting with a care provider about the next steps to ensure your and your loved ones' safety after receiving therapy. He also recommends exploring resources and information about radioactive iodine therapy provided by the American Thyroid Association.
Although radioactive iodine therapy has been used to treat humans for nearly a century, Peters says ongoing research continues to seek to optimize the therapy’s effectiveness and patient experience by assessing dose strategies and reduction of side effects.
“Our care teams are happy to be able to offer radioactive iodine therapy and guide patients through the process to prolong and improve their quality of life," Peters says.
Care teams at Loma Linda University Cancer Center have treated countless patients with thyroid cancers or disorders over decades using radioactive iodine therapy. Learn more about the Cancer Center’s thyroid cancer services and treatment options online or call 1-800-782-2623 to make an appointment.


