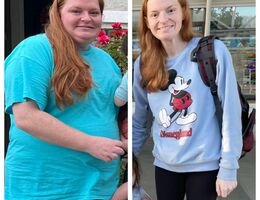
Sleeve gastrectomy removes 80% of the stomach, leading to substantial weight loss
The gastric sleeve procedure — known medically as a sleeve gastrectomy — is one of the most performed bariatric weight loss surgeries in the United States. According to Keith Scharf, DO, FACS, FASMBS, a bariatric surgeon at Loma Linda University Health, the procedure focuses entirely on the stomach.
“About 80 to 85 percent of the stomach is stapled and removed,” Scharf explains. “The operation usually takes about an hour, is performed in a minimally invasive approach with several small incisions, and is typically a one-night hospital stay.”
Patients are able to walk the same day of their surgery and start a liquid diet shortly after waking up from anesthesia.
Why gastric sleeve procedure is more than just a weight loss surgery
A sleeve gastrectomy is more than simply making the stomach smaller. While surgery reduces stomach size and helps to limit how much food a person consumes, Sharf says the primary effects are metabolic.
“There are significant changes in gut hormones and brain chemistry after surgery. Patients often notice differences in appetite, taste, smell, and how quickly they feel full,” Scharf says.
This change between the gut and the brain helps patients feel satisfied after eating smaller portions, with many reporting a dramatic reduction in appetite altogether. Compared to GLP1s, which are known to quiet food noise, if a patient were to stop taking their medication, that food noise would come back. Hormonal change from the gastric sleeve helps to alter the way the brain thinks about food altogether, reducing or stopping food noise entirely.
Additionally, bariatric surgery can increase metabolic expenditure, helping the body burn calories more efficiently.

Surgery and recovery
Before surgery, patients are typically given weight-loss goals through a comprehensive bariatric program that includes nutrition classes, consultations with dietitians, appointments with mental healthcare professionals, and lifestyle education as a vital part of preparation.
The importance of these mandatory classes is not just to prep a patient for surgery, but also to help shift their mindset for life after weight loss.
“Surgery is the most powerful tool we have to treat obesity, which is a chronic illness, but it only works if patients are committed to long-term lifestyle changes,” Scharf says.
Pre-operative goals help patients start adjusting their eating habits, activity levels, and mindset before surgery. They also ensure patients are ready for the lifelong changes that follow.
Once a patient completes their pre-surgery program and undergoes surgery, recovery is relatively quick. Patients begin with a clear liquid diet in the hospital, followed by a full liquid diet at home for about two weeks. From there, they gradually progress to puréed foods, soft foods, and eventually solid foods by about six weeks post-surgery.
“The progression isn’t about restriction. It’s about learning how to eat again,” Scharf says.
Eating too quickly or too much too soon can cause nausea, discomfort, or vomiting. The staged diet allows the body to adapt and helps patients understand their new sensations of hunger and fullness.
Weight loss after a gastric sleeve procedure
Weight loss after gastric sleeve is fastest during the first six months, but it continues gradually over time, with Scharf saying most patients plateau between 12 and 18 months after surgery.
“Rather than focusing solely on pounds lost, clinicians often measure success by percentage of total body weight or excess body weight loss. On average, sleeve gastrectomy patients lose about 60 to 65 percent of their excess body weight within the first year to year and a half,” Scharf explains.
Importantly, weight loss is not linear. Plateaus are normal, and brief stalls do not mean failure.
When to consider weight loss surgery
Current guidelines generally recommend bariatric surgery for individuals with a body mass index (BMI) of 40 or higher, or a BMI of 35 or higher with obesity-related medical conditions such as diabetes, high blood pressure, or sleep apnea.
Repeated cycles of weight loss and regain are common in patients suffering from obesity, driven by powerful biological mechanisms that increase hunger and slow metabolism after weight loss.
“If patients meet the criteria and have tried other approaches without long-term success, surgery can be an important option,” Scharf says.
Anyone suffering from obesity or other medical conditions related to obesity, such as type II diabetes, sleep apnea, high blood pressure, or high cholesterol, might be a candidate for sleeve gastrectomy or other weight loss surgeries. For more information, call us at 909-651-7091 or visit our website here.