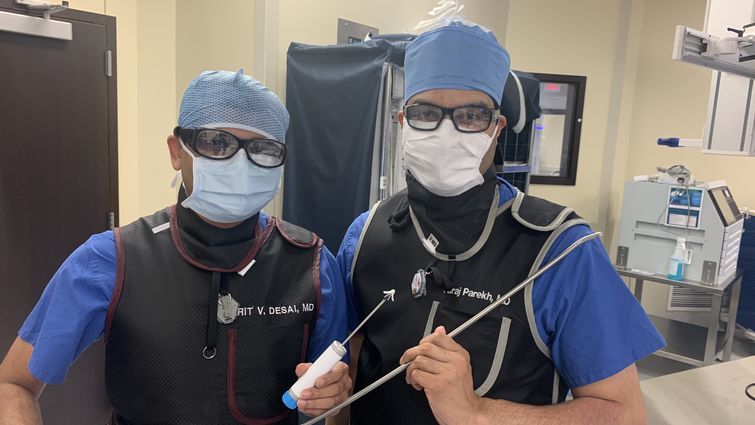
From left, cardiologists Harit Desai, MD, and Niraj Parekh, MD, hold surgical equipment used to repair patients’ heart valves during TMVr — a procedure that saved Elenita Tan’s life in December 2020.
Elenita Tan’s organs were failing, and as physicians at Loma Linda University Medical Center – Murrieta faced a true do-or-die situation, they opted to perform a transcatheter mitral valve repair (TMVr) procedure that ultimately saved the 83-year-old woman’s life.
By the time Tan arrived at the hospital, she was suffering from acute congestive heart failure, said Harit Desai, MD, the associate director for the cardiac catheterization lab and structural heart intervention program at LLUMC – Murrieta. Before long, Tan experienced multi-organ system failure, placing her at high risk for serious and possibly lethal complications.
“I really didn’t think I was going to make it,” said Tan, who worked as a registered nurse in both New York and California but had never before set foot in a hospital for her own health concerns — the exception being the birth of her children.
Desai and other physicians in the structural heart team deemed Tan ineligible for open-heart surgery because of high surgical risk and the demanding strain it would place on her body with faltering organs.
The TMVr procedure was the last chance to repair the valve and hopefully reverse the multi-organ failure.Dr. Harit Desai
Instead, the team set out to deliver a less-invasive procedure, TMVr, to repair Tan’s failing mitral valve. The operation involves the insertion of a thin wire through a large vein in the patient’s leg in order to access the heart. Surgeons guide a small MitraClip device up the leg vein that clips together an area of the heart valve. While the valve continues to open and close on either side of the clip, blood continues to flow on both sides, reducing backward flow.
It had become apparent to Tan that something was amiss with her heart health when simple tasks such as walking short distances, brushing her teeth and even chewing food left her breathless. As a retiree who still actively traveled abroad and volunteered on surgical mission trips in the Philippines, Tan said the sudden change in pace was alarming.
Because of her condition, Tan said she endured sleepless nights and made multiple calls to her doctor who could not see her because her incessant coughing sounded like a symptom of COVID-19. She was finally able to see her primary care provider and then a cardiologist, who scheduled an echocardiogram test. Upon reviewing the test results, the cardiologist immediately rushed her to the Murrieta hospital for intervention.
She was diagnosed with flail mitral leaflet, meaning the flaps in one of her heart valves tore away from her heart muscle and lost the ability to keep blood from flowing backward in the lungs.
“The TMVr procedure was the last chance to repair the valve and hopefully reverse the multi-organ failure,” Desai said.
 Tan underwent the procedure in late December 2020. She is now at home recovering and says she is better able to breathe and sleep. Desai said skilled cardiac anesthesiologists were able to account for Tan’s already very low blood pressure going into surgery and administer medication accordingly to avoid risk of cardiac arrest.
Tan underwent the procedure in late December 2020. She is now at home recovering and says she is better able to breathe and sleep. Desai said skilled cardiac anesthesiologists were able to account for Tan’s already very low blood pressure going into surgery and administer medication accordingly to avoid risk of cardiac arrest.
“The combination of expertise and teamwork between surgeons and anesthesiologists is what enhances the structural heart disease program,” Desai said. "Our team has built a track record of successfully treating patients with this innovative piece of technology, and we've been able to dramatically improve the health and quality of life for many patients who couldn’t have been helped or would have had to go through open-heart surgery with all of its attendant risk."
Since performing the first TMVr procedure in the region, physicians at LLUMC — Murrieta have completed 100 procedures. 72-year-old Murrieta resident Linda Williams became the 100th patient to undergo TMVr at Murrieta as of March 8. Desai says technology for the procedure continues to grow more refined and allows for personalized care, as the clip devices now come in customized lengths and widths to best meet the patient’s need.
Compared to open-heart surgery, a TMVr procedure to repair a mitral valve offers reduced surgical risk, less bodily invasion, and shortened recovery time. A recent study reports about 50% of patients who undergo TMVr require less future hospitalizations for heart failure, and it reduces the risk of mortality by 30%.
Desai said it is key to be vigilant for symptoms of a failing heart valve and catch them early. These include shortness of breath, swelling in feet, inability to exercise or to maintain activity that was once routine six months ago, and fatigue. Should you experience these symptoms, do not delay speaking with your primary care provider or cardiologist about treatment. Delaying care can lead to the development of life-threatening conditions, which are more difficult to treat, he said.
To learn more about TMVr and heart care services at Loma Linda University Medical Center — Murrieta, visit their murrieta.lluh.org/services/heart-vascular or call 951-290-4314.

