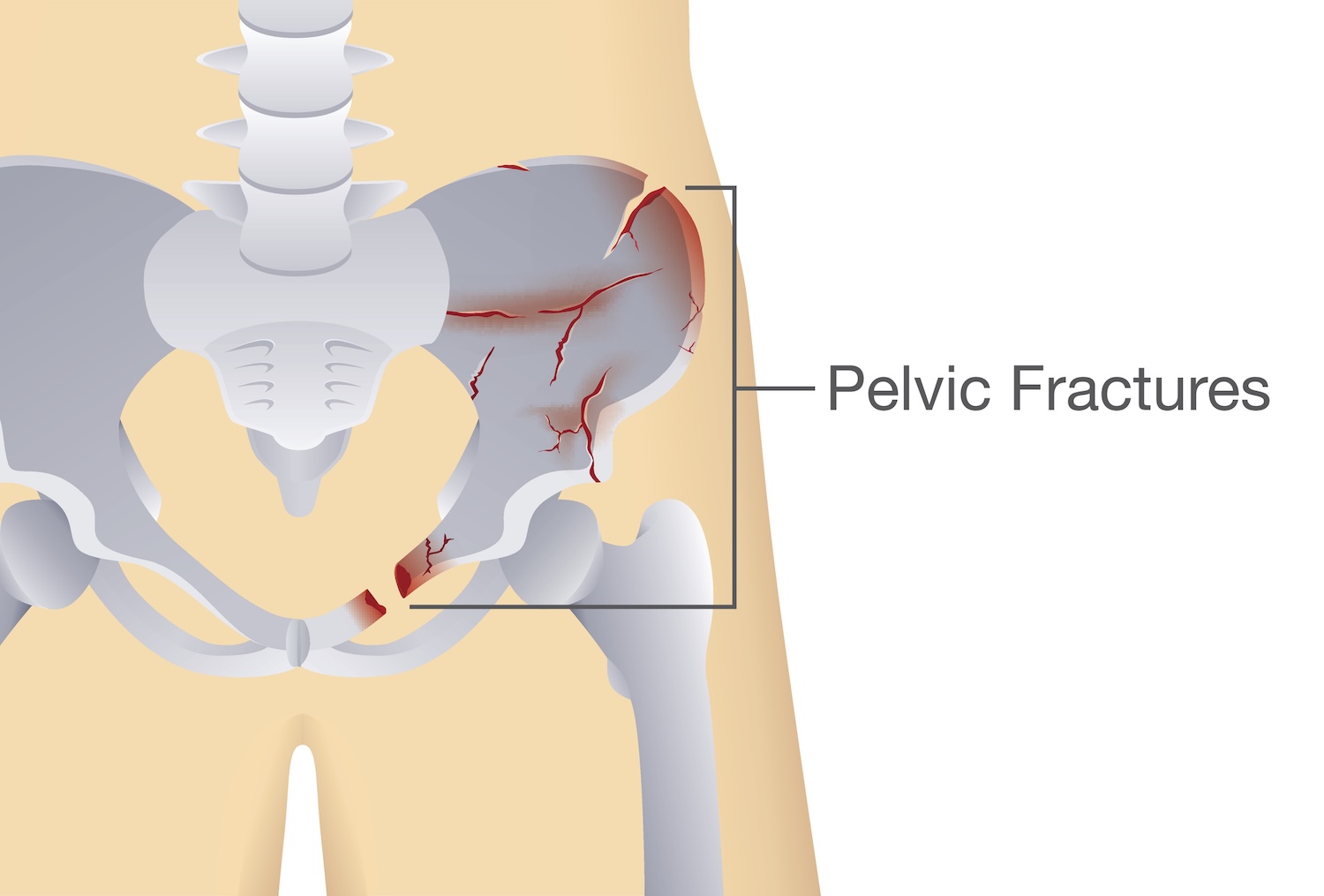

Adults over the age of 65 are at risk of a pelvic fracture from a low-energy fall
As we age, bones naturally become weaker, reaction time slows, and balance issues become more common, all of which increase the risk of falling. Geriatric pelvic fractures are among the most common fall-related injuries in older adults.
While often mistaken for hip fractures, Jessica Kingsberg, MD, an orthopaedic surgeon at Loma Linda University Health, notes that these injuries are distinct and require a different approach to treatment.
“A geriatric pelvic fracture is a break in one or more of the bones that make up the pelvis —the ring of bones located just above the hip,” Kingsberg explains.
“These fractures typically occur in patients over the age of 65 and are usually the result of a low-energy injury, most commonly a fall from standing height.
Unlike younger patients, whose pelvic fractures usually result from high-energy trauma such as car accidents or major falls, older adults can sustain pelvic fractures from something as simple as losing their balance and landing on their side. Age-related bone loss, muscle weakness, dizziness, and balance problems all contribute to the growing number of pelvic fractures seen in older adults.
What happens after falling?
After a fall, most patients are taken to the hospital for imaging and evaluation. One of the most important factors in determining treatment is whether the patient can walk.
“If a patient is still able to walk, the injury is considered stable, meaning the broken bones are unlikely to shift or worsen,” Kingsberg says.
These patients can often bear weight safely and begin physical therapy, typically using a walker for support. If walking is not possible, the injury is more complex, and treatment decisions become more involved.

Geriatric pelvic surgery
For injuries requiring more than physical therapy and time to heal, surgery may be beneficial, especially if there are multiple fractures. Fortunately, the procedure is quick —typically about one hour — minimally invasive, and involves little blood loss, making it safer for older patients than more extensive surgeries.
“Surgeons use small incisions and screws to stabilize and reinforce the bone, helping keep the pelvis secure while it heals,” Kingsberg says.
After surgery, patients are allowed to put full pressure on their leg as tolerated. While pain may still be present, patients are encouraged to move and usually use a walker for about six weeks, with most feeling close to normal by three months.
While surgery can be intimidating, Kingsberg warns that avoiding it may prolong pain and delay recovery.
“Patients who undergo surgery when it’s recommended often have better outcomes because they walk sooner and have better pain control.”
Preventing pelvic fractures
Prevention starts with understanding bone health. A DEXA scan, which measures bone density, can identify osteoporosis or low bone mass. While commonly recommended for women after menopause, bone density screening can be valuable for anyone at risk.
Reducing fall risks is equally important. This includes:
-
Addressing dizziness or balance problems promptly
-
Removing tripping hazards like loose rugs
-
Keeping walkways clear
-
Using canes or walkers when needed
For more information, visit our website here.