Loma Linda University Children’s Hospital is now home to the Tiny Baby Program (TBP), providing unique, specialized care for very small babies born at 28 weeks’ gestation or earlier and weighing less than 1,000 grams or 2.2 pounds.
A formal ribbon-cutting ceremony was held on Monday, Oct. 8 celebrating the program and the 45th anniversary of the neonatal intensive care unit (NICU) at Children’s Hospital.
A ‘sacred place’
As part of the 84-bed NICU, the designated Tiny Baby Unit has 12 beds within a separate space that was specially designed to care for these fragile babies. An additional 12 beds within the main NICU serves as an extension of this program.
Anamika Banerji, MD, MS, a neonatologist and medical director of the Tiny Baby Program, says the babies in these rooms are protected from excessive light and sound in an effort to make the environment more similar to what they would be experiencing inside mother’s womb if they had not been born so prematurely. Babies are also provided soft positioning aids inside their incubators to support the tucked, flexed position they would have been inside the womb.
“It’s a sacred space,” Banerji said. “We are trying to provide the best medical care possible outside the mother’s womb while also trying to mimic aspects of the environment the baby would be developmentally expecting.”
We know parents are the most important people in a baby’s life and recognize them as vital members of the care team. Raylene Phillips, MD
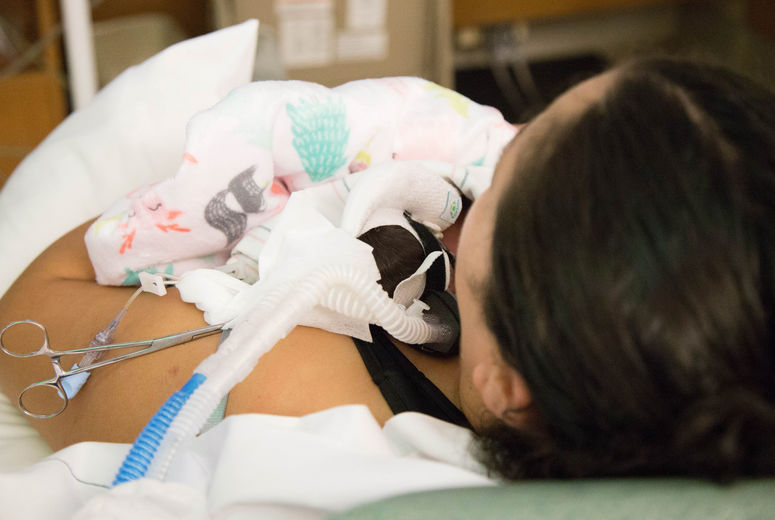
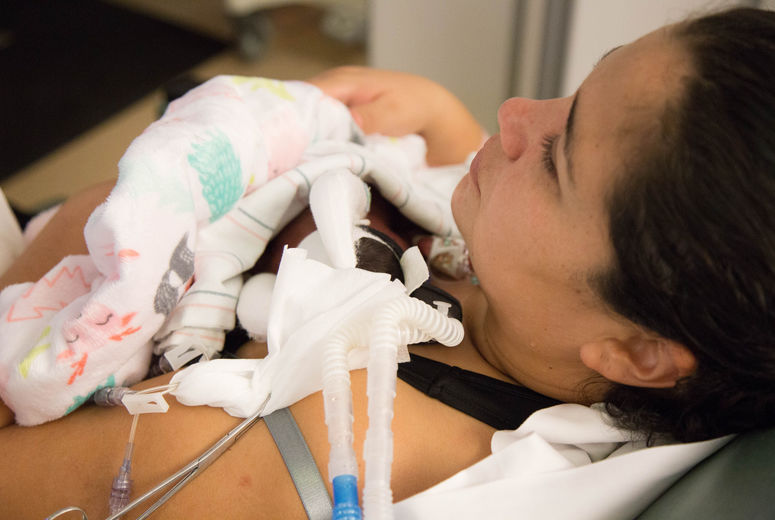
Raylene Phillips, MD, MA, an infant developmental specialist and neonatologist who worked with Banerji in developing the Tiny Baby Program, said they are emphasizing skin-to-skin contact with the baby’s mother when medically possible, pointing out that studies have shown that premature infants are usually most stable when they are in contact with their mothers or fathers, who are also encouraged to hold their babies skin to skin.
“We know parents are the most important people in a baby’s life and recognize them as vital members of the care team,” Phillips said.
There are nearly 500,000 babies born every year in California, and approximately 1.4 percent are born at extremely low birthweight — less than 1000 grams, or 2.2 pounds according to the March of Dimes. These babies, born several months prematurely, must continue their development outside the womb.
Breathing before their lungs are fully mature and being exposed to different levels of noise and sound stimuli than they would have experienced inside the womb creates challenges as they grow and develop, including increased risk for chronic lung disease, hearing loss, learning disabilities, behavioral and social abnormalities, and accentuated sensitivities to touch or pain. Their fragile brains are also more susceptible to injury, which can lead to cerebral palsy.
According to Banerji, the consequences of extreme prematurity can impact these babies for the rest of their lives.
“Our goal is to improve survival and decrease the severity and frequency of these serious lifelong conditions,” Banerji said. “In addition to providing excellent medical care, we make every effort to help these tiny babies feel safe, supported, and connected to their parents because we know this helps them better cope with many of the stressful or painful experiences they may have to endure while in the NICU.
What makes the Tiny Baby Program unique
Two-person, four-handed care. Any time the infant needs to be touched or handled, two people and four hands are always used. One person will hold or cradle the baby in a flexed position as if still in the womb, while the other person will complete the caregiving task (such as a diaper change) or procedure needed. Providing this level of support helps the baby to remain physiologically stable during the care or procedure.
Structured interdisciplinary bedside rounds (SIBR). This is a way of doing “rounds” where critical information about the patients’ plan of care is discussed each morning among the care team. In this model, the entire multidisciplinary team meets together to share information and create and implement care plans. This allows for more effective communication and more efficient rounds.
Banerji said she and her team created templates that allow staff to know what information to report and discuss for each patient. Each member of the team plays a vital role and has an investment in the plans developed together.
“When every member of the team has a stake or investment, people are excited about the collaborative effort. We believe these efforts will results in better care and enable babies to go home sooner and healthier,” Phillips said.
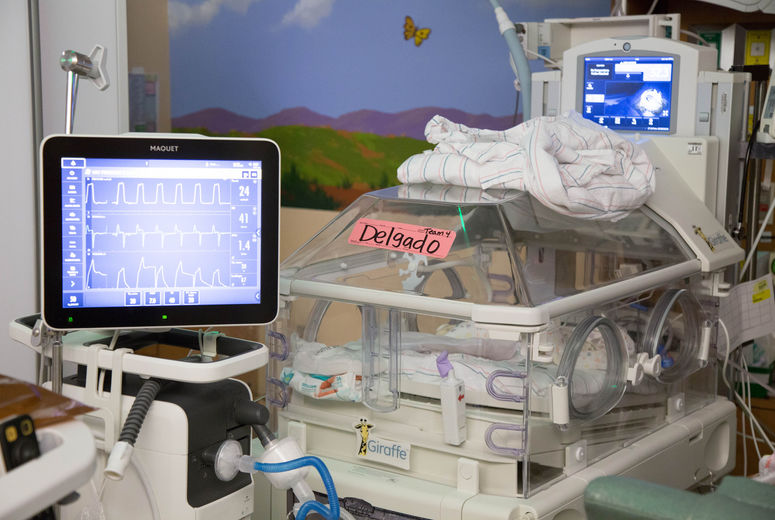
Standardized protocols and cutting-edge technology. The TBP emphasizes the use of standardized protocols based on the most current medical evidence to optimize good outcomes in these babies. This includes maximizing nasal ventilation, also known as non-invasive respiratory support, and minimizing the use and duration of breathing tubes to decrease the risk of developing chronic lung damage.
The TBP also uses new technology to monitor and manage these fragile babies. The use of near infrared spectroscopy (NIRS) monitoring allows for non-invasive, continuous measurement of oxygen levels in the brain, kidneys and the gastrointestinal tract. It is used as an additional vital sign to ensure adequate tissue oxygen saturation and perfusion to these organs and minimize brain injury in these babies.
Although there are other small baby programs in California and other states, the Tiny Baby Program is the only one of its kind in the Inland Empire. It involves a multidisciplinary team of specially trained physicians, nurses, respiratory care practitioners, physical/occupational therapists, nutritionists, pharmacists, child life specialists, case managers, and, of course, parents.
A proactive approach for better outcomes
The program begins even before a baby is born and continues after discharge.
At Loma Linda University Children’s Health, obstetricians and neonatologists work together to consult with expectant moms who are faced with the possibility of their baby being born prematurely.
“Parents aren’t usually prepared for that,” Banerji said. “But it’s important to review potential challenges when preparing to deliver a premature or sick baby so that outcomes are optimized.” Tiny babies who graduate from the NICU are followed in the high-risk infant follow-up clinic to assess their physical and developmental milestones.
Tiny baby outcomes have improved, Banerji said. Tiny babies today are able to go home sooner and with healthier lungs. “These tiny babies are thriving because of how we are caring for them. With more time, we hope to be able to show significant improvement in both survival and reduction in the serious sequelae of prematurity.”
Parents feel like they’re taking home a miracle, and it’s an incredible feeling to know that we were a part of that. Anamika Banerji, MD
Banerji feels blessed to have had the opportunity to help develop the Tiny Baby Program and to move it forward. “We are all a part of a large team, each member of whom puts forth so much effort and heart for the care of these fragile babies.”
“We are seeing a difference,” she said. “Parents feel like they’re taking home a miracle, and it’s an incredible feeling to know that we were a part of that.”
For more information about the Tiny Baby Program or the NICU at Loma Linda University Children’s Hospital, visit lluch.org or call 800-825-KIDS.